Your Revenue Cycle Is Leaking Cash, and Your Billing Codes Are Why
The agentic AI is the game-changer
The Revenue War Nobody Told You
Revenue codes are a strategic asset, not just billing
Agentic AI turns denial prevention into proactive wins
Siloed data is the silent killer of AI adoption
Underpayment detection delivers the highest hidden ROI
How agentic AI is finally turning revenue code data from a compliance headache into a margin-generating machine - and what you need to do about it today.
If you are running the revenue cycle for a US health system right now, you already know the walls are closing in. Payer denial rates are climbing. Operating margins are thinning. Your finance team is buried in spreadsheets that tell you what went wrong last quarter, not what is going wrong this morning.
And somewhere in the middle of all that noise, your revenue code data sits quietly inside static billing reports, doing almost nothing to protect your bottom line.
This is not a technology problem. It is a strategy problem. Here is what the data is telling us, what your peers in healthcare finance are already starting to do about it, and how the right AI infrastructure can finally turn that billing data into a real-time margin lever.
The Payer Denial Crisis That Is Already Draining Your Operating Margins
Let us be direct about something: the denial environment has shifted structurally, not temporarily. Payers are deploying increasingly sophisticated analytics and automation to scrutinize claims at a level your current tools were never designed to match. Revenue code data - those three- and four-digit numeric codes that describe the type of service delivered on every institutional claim - sits at the center of that battle. And most organizations are still treating that data like a compliance checkbox rather than the strategic signal it actually is.
As health systems prepare for higher denial rates, stricter payer policies, and ongoing pressure on operating margins, CFOs are being asked to protect earnings and fund strategic growth with increasingly limited resources. Many organizations have already invested in automation, but their revenue code data remains trapped in static reports and retrospective audits that do little to improve current-year performance. The problem compounds every billing cycle.
The financial consequences are not abstract. Denial rate spikes translate directly into delayed cash flow, increased days in accounts receivable, and write-offs that stack up quarter after quarter. If you are not treating revenue code data as a real-time signal for denial risk and missed revenue, you are already behind the curve - and the gap is widening faster than most finance leaders realize.
Your data is already the asset. The right platform turns it into action.
DataManagement.ai is purpose-built to help healthcare finance and revenue integrity teams structure, govern, and activate their revenue code data through AI - so you stop reacting to denials and start preventing them before they cost you another dollar.

The Billing Code Blind Spot That Is Costing You Millions
If you have been thinking about revenue codes primarily as a billing artifact, you are leaving significant strategic value sitting untouched. Every revenue code connects the clinical work your teams performed to the reimbursement you are contractually owed.
It carries embedded information about care intensity, service setting, payer-specific contract terms, documentation patterns, and coding practices - all compressed into a single, machine-readable data point.
AI-driven revenue cycle management works best when you combine human expertise with AI to drive informed decision-making and efficiency. But that combination only performs at scale when the underlying data is structured, clean, and connected to the right clinical and financial context. Most health systems right now are sitting on a gold mine of revenue code data; they are not fully equipped to activate.
When you treat revenue codes as strategic signals rather than billing artifacts, three capabilities open up immediately. First, you can identify denial risk far earlier - by payer, by service line, and by specific code combinations - giving your team the window it needs to intervene before a claim goes out the door.
Second, you can pinpoint the encounters where your charges are routinely under-captured, miscoded, or downgraded, and put a precise dollar figure on what that costs you annually. Third, you can model cash flow and net collection rates with real code-level granularity, rather than depending on lagging indicators that reflect conditions from three months ago.
Traditional business intelligence reports cover last quarter's events. Agentic AI uses the same revenue code data to prevent issues like missed charges, underpayments, and avoidable denials from occurring in the first place. That shift - from descriptive reporting to active prevention - is where the actual margin opportunity lives, and it is available to you right now.
AI Is Changing What Healthcare CFOs Can Do. Here Is Proof.
The conversation around AI in revenue cycle management has matured sharply. You are no longer evaluating whether to use AI. The real question is which use cases you prioritize first, and whether your data infrastructure can support the agents you are trying to deploy at scale.
AI use in the healthcare revenue cycle is now touching all areas of administrative and financial operations, improving overall productivity and translating directly into monetary gains for the sector. But some applications are already delivering measurable results while others remain aspirational. Here is where the leading organizations are investing their focus right now.
Denial prevention is the highest-impact starting point for most systems. An AI agent trained on payer-specific denial patterns can flag at-risk claims in real time, recommend documentation addenda or code adjustments, and trigger preemptive action before submission.
Research consistently shows that predicting potential denials before submission saves time and enables faster resolution with significantly less revenue leakage. That is not incremental improvement - it is a fundamentally different operating model for your revenue integrity team.
Underpayment detection is the second high-value use case that most organizations are significantly underfunding relative to its actual return. The gap between what your contracts entitle you to and what you actually receive is often larger than any CFO wants to admit, and it compounds across thousands of claims every quarter.
An AI agent that systematically compares expected reimbursement by contract and revenue code structure against actual payments can surface patterns of systematic underpayment that your current team simply does not have the bandwidth to catch manually.
Pre-bill revenue integrity - scanning every claim for missing charges, mismatched revenue code and HCPCS combinations, and absent modifiers before submission - is a third area where agentic AI has already proven measurable value in live health system deployments.
When that work is done by an AI agent rather than a human reviewer, it happens faster, more consistently, and at a volume no manual process can sustain. Your staff capacity shifts from routine claim review to complex, high-value case resolution - which is exactly where experienced team members should be focused.
By drawing on real-time analysis of historical claims data, AI enhances work queue optimization, forecasts better claim outcomes, and recommends more strategic resource allocation across the revenue cycle. That combination of speed, scale, and specificity separates organizations that are capturing measurable margin gains from those still running pilots that never convert to production.
AI Adoption Is Failing Most Health Systems. Here Is Why.
Knowing what AI can do and actually capturing that value in production are two very different conversations. The gap between them is where most organizations stall, and if you have been frustrated by slow progress on AI adoption, there are predictable reasons for it.
The most common starting point for failure is data quality and integration. Legacy systems have limited interoperability, making it genuinely difficult to connect EHR platforms and billing systems to AI-driven tools without introducing data quality problems. If your revenue code data is siloed across inpatient, outpatient, ED, and post-acute settings without a unified, governed data layer underneath it, your AI agents are operating on incomplete information - and incomplete information produces inconsistent outputs that erode trust quickly.
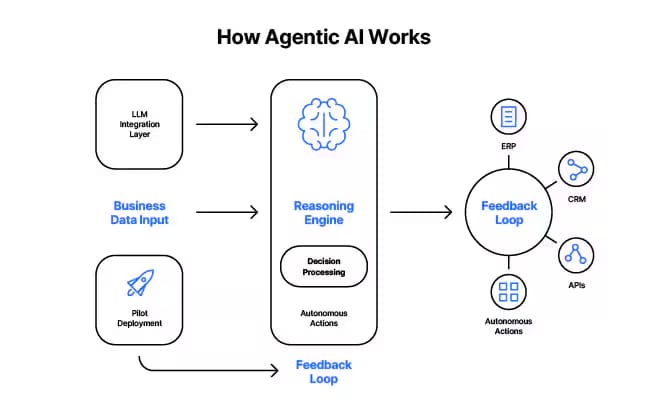
Capital investment is a real constraint that does not get acknowledged enough in vendor conversations. Training teams on new frameworks, redesigning workflows to accommodate AI recommendations, and building compliance and governance infrastructure around autonomous agents all carry costs that must be weighed carefully against expected ROI. Many healthcare organizations slow down or limit AI adoption for exactly this reason, and it is a legitimate concern.
Compliance is the third barrier that rarely gets the attention it deserves. Revenue code decisions directly influence reimbursement and regulatory exposure. Every AI agent operating in this space needs transparent logic, clear audit trails, and meaningful human oversight mechanisms - not because AI cannot be trusted, but because your compliance, legal, and HIM teams need to be able to stand behind every output the system produces.
While AI can substantially accelerate operational speed through automation, achieving optimal results requires combining automation with genuine human oversight. The organizations winning this game have built that human-AI collaboration model intentionally, with clear accuracy thresholds, structured feedback loops, and governance councils that include compliance, clinical, and revenue integrity leaders working toward the same objectives.
On the payer and reinsurance side of the equation, the same claims data driving your denial problem is creating financial exposure that most current tools were never built to catch.
Reinsured.ai brings AI-powered intelligence to claims review, helping payers and reinsurers identify pricing discrepancies, underpayments, and financial risk at the line-item level - before they become material balance sheet problems that surface at the wrong moment.

The AI Playbook Your Competitors Are Running While You Wait
The health systems seeing real, auditable results from AI in the revenue cycle share a set of characteristics worth studying closely. They did not start by purchasing software and expecting transformation to follow automatically. They started by treating their revenue code data as a strategic asset that needed to be governed, cleaned, and contextually connected before any intelligent agent could use it effectively.
They also started small on purpose. Rather than attempting system-wide AI deployment all at once, they selected two or three high-value use cases - typically in service lines with the highest denial rates and the most payer scrutiny - and committed to demonstrating measurable financial impact within a defined six-to-twelve-month window. That discipline builds organizational confidence and creates a replicable playbook for scaling.
The organizations that succeed in this next phase will blend deep subject-matter expertise with intelligent agents, using revenue code data as the shared language among clinicians, operators, and machines. This is not an IT initiative. It is a financial transformation initiative that uses AI as the engine.
The question for your organization is not whether this shift is happening. It is whether you are positioned to lead it or spend the next three years catching up to the systems that moved first. Your revenue code data already contains the signals you need to drive better denial rates, faster cash flow, and stronger net collection. The platforms to activate those signals are operational, proven, and live right now.
The margin advantage goes to whoever moves first.
Your revenue code data is already telling you where the money is leaking. The right data management platform just helps you listen in real time before another billing cycle slips by.

Warm regards,
Shen and Team